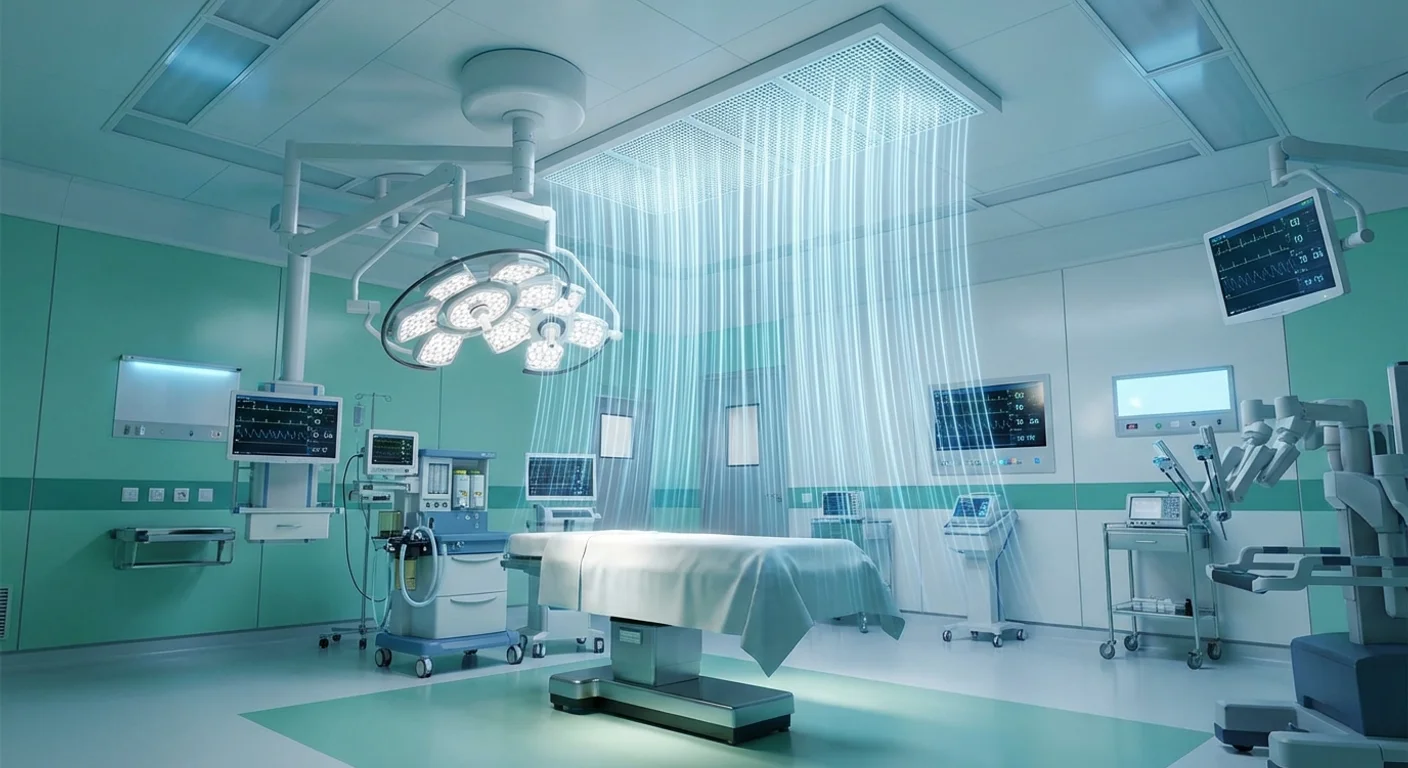
The operating room (OR) is the most stringently controlled environment in healthcare facilities. The HVAC system plays a role far beyond simple temperature regulation — it is a core engineering measure for preventing Surgical Site Infections (SSI). According to the U.S. Centers for Disease Control and Prevention (CDC), SSI incidence rates are approximately 2-5%, with airborne particulate being a significant infection pathway[1]. This article systematically analyzes the core design parameters for operating room HVAC, laminar flow system design principles, and Taiwan's regulatory requirements, starting from ASHRAE Standard 170 and international design guidelines, providing rigorous design references for healthcare facility construction projects. For a general overview of healthcare HVAC, please refer to our article on Hospital HVAC System Design.
1. Regulatory Foundation for Operating Room HVAC Design
The international authoritative reference for OR HVAC design is ANSI/ASHRAE/ASHE Standard 170 — Ventilation of Health Care Facilities. This standard, jointly developed by ASHRAE and the American Society for Healthcare Engineering (ASHE), specifies ventilation, pressure relationships, temperature and humidity, and air filtration requirements for various types of healthcare spaces[2].
In Taiwan, operating room HVAC design primarily follows these regulations and guidelines:
- Ministry of Health and Welfare "Standards for Medical Facility Establishment": Specifies basic facility requirements for operating rooms, including HVAC, lighting, and emergency power[3]
- Ministry of the Interior "Building Technical Regulations" — Building Equipment Chapter: General provisions for building mechanical ventilation and HVAC equipment
- FGI "Guidelines for Design and Construction of Hospitals": American healthcare facility design guidelines, used as design reference by many medical centers in Taiwan[4]
2. ASHRAE 170 Operating Room Design Parameters
ASHRAE Standard 170-2021 Table 7-1 explicitly specifies the environmental design parameters for operating rooms[5]:
| Parameter | Standard Requirement | Notes |
|---|---|---|
| Pressure Relationship | Positive (≥ +2.5 Pa) | Relative to corridors and adjacent non-clean areas |
| Total Air Changes | ≥ 20 ACH | Existing facilities minimum 15 ACH |
| Outdoor Air Changes | ≥ 4 ACH | Ensures indoor air quality |
| Temperature Range | 20–24°C | Adjustable per surgical needs (e.g., lower for cardiac surgery) |
| Relative Humidity | 20–60% RH | 2021 edition lowered minimum from 30% to 20% |
| Air Filtration | At least two-stage filtration | MERV 7 + MERV 14 (minimum) |
| Return Air Restriction | No shared return air with other areas | OR return air must not mix with other zones |
Engineering Significance of Positive Pressure Control
The purpose of maintaining positive pressure in the operating room is to ensure that the airflow direction when the door opens is "from the OR toward the corridor," preventing contaminated air from the corridor from entering the surgical area. Positive pressure ≥ +2.5 Pa is a dynamic equilibrium — when the OR door is closed, the pressure differential should stabilize at +5 to +15 Pa; when the door opens, the supply air volume must be sufficient to maintain continuous outward airflow despite the momentary pressure differential release. In practice, the difference between OR supply air volume and return air volume (i.e., the overflow air volume) is recommended to be maintained at 200-400 CFM[6].
3. Laminar Flow vs. Turbulent Flow Operating Room Design
Based on airflow organization, operating rooms can be classified into "laminar flow ORs" and "turbulent flow ORs." The two differ significantly in particulate control capability, cost, and applicable scenarios[7].
Laminar Flow Operating Room (Unidirectional Airflow OR)
A laminar flow OR features a large-area HEPA-filtered supply air ceiling (Laminar Airflow Canopy) installed directly above the operating table, typically measuring 2.4m x 3.0m or larger, covering the operating table and primary instrument area. Clean air is blown vertically downward at a uniform velocity of 0.2-0.3 m/s, continuously pushing particulates away from the surgical area into low-level return air outlets around the periphery[8].
Laminar flow ORs can achieve ISO Class 5 cleanliness (equivalent to the former Fed-Std-209E Class 100), suitable for:
- Total Joint Replacement surgery
- Organ transplant surgery
- Cardiac surgery
- Neurosurgery
Design must account for the interference of surgical lights on the airflow field. Traditional large surgical lights create wake effects on the downwind side, forming particulate retention zones. Modern surgical lights adopt airflow-compatible designs to reduce laminar flow disturbance[9].
Turbulent Flow Operating Room (Non-Unidirectional Airflow OR)
Turbulent flow ORs use multi-point ceiling supply with low-level return air in a mixed airflow pattern, achieving particulate dilution through high air change rates (≥ 20 ACH). Their cleanliness level is approximately ISO Class 7-8, suitable for general surgery, obstetrics and gynecology, ophthalmology, and other non-implant procedures. Turbulent flow OR construction costs are approximately 60-70% of laminar flow ORs, with lower maintenance costs as well[7].
4. HEPA Filtration System Configuration
Operating room air filtration employs a multi-stage series architecture[10]:
- First Stage (Pre-filtration): MERV 7-8, installed at the AHU intake, intercepting large-diameter dust and protecting downstream filters
- Second Stage (Medium-efficiency filtration): MERV 14-16, installed in the AHU supply air section, intercepting 0.3-1.0 μm particulates
- Third Stage (Terminal filtration): HEPA H13 (efficiency ≥ 99.95% @ 0.3 μm) or H14 (efficiency ≥ 99.995% @ 0.3 μm), installed in the OR ceiling supply air panels as the final barrier
HEPA filter pressure drop management is a maintenance priority. New filters have an initial pressure drop of approximately 120-250 Pa; as pressure drop increases with use, replacement is required when it exceeds the terminal value (typically 2x the initial pressure drop). The HVAC control system should include differential pressure sensors and provide replacement alerts.
5. Clinical Considerations for Temperature and Humidity Control
Temperature and humidity settings in operating rooms are not merely comfort considerations but are directly related to surgical safety:
- Lower Temperature (20-22°C): Beneficial for reducing the thermal load on surgical teams wearing isolation gowns, but care must be taken as anesthetized patients are susceptible to hypothermia, which increases post-operative infection risk. ASHRAE 170 allows physicians to adjust temperature as needed[11]
- Low Humidity (<20% RH): Increases electrostatic discharge (ESD) risk, potentially interfering with electronic medical instruments; also dries respiratory mucous membranes, hindering patient recovery
- High Humidity (>60% RH): Promotes microbial growth, unfavorable for surgical site dryness, and increases the risk of surgical instrument oxidation and corrosion
In Taiwan's subtropical climate with high outdoor humidity, the dehumidification capacity of OR HVAC systems is particularly critical. A dedicated outdoor air handling unit (DOAS) is recommended to pre-cool and dehumidify outdoor air to a dew point of 8-10°C before mixing it with the OR air handling unit supply.
6. Bridging Taiwan Regulations and International Standards
Taiwan's Standards for Medical Facility Establishment provides relatively general provisions for OR HVAC. In practice, most medical centers use ASHRAE 170 and FGI Guidelines as their design basis. Several noteworthy localization issues include:
- Hospital Accreditation: In the Ministry of Health and Welfare's hospital accreditation criteria, OR environmental management is an evaluation focus, covering HVAC system maintenance records, temperature and humidity monitoring, and filter replacement records[12]
- Infection Control Inspections: The Centers for Disease Control's healthcare facility infection control inspections include OR HVAC positive pressure verification and particulate monitoring
- Seismic Resilience: As Taiwan is located in a seismically active zone, seismic restraint design for OR HVAC ductwork and equipment must comply with the Building Technical Regulations' seismic requirements
Conclusion
Operating room HVAC design is one of the most technically demanding specializations in healthcare building engineering. From positive pressure control to laminar flow design, from HEPA filtration to precision temperature and humidity control, every design parameter represents a rigorous commitment to surgical safety. As refrigeration and HVAC engineering professionals, we consistently adhere to ASHRAE 170 and FGI Guidelines as our design foundation for OR projects, combining Taiwan's local regulations and climate conditions to create reliable clean surgical environments for medical teams.